 Urinary tract infections (UTIs) are common in kids. By age 5, about 8% of girls and 1%-2% of boys have had at least one UTI. They occur when the kidneys, ureters, bladder, or urethra
Urinary tract infections (UTIs) are common in kids. By age 5, about 8% of girls and 1%-2% of boys have had at least one UTI. They occur when the kidneys, ureters, bladder, or urethrabecome infected.
Symptoms of a UTI can include:
- pain when urinating
- changes in frequency, appearance, or smell of urine
- fever
- chills
- loss of appetite
- nausea
- vomiting
- lower abdominal pain
- lower back pain or discomfort
UTIs can also cause bedwetting in kids who were previously dry at night. Infants and young children may only show nonspecific signs such as fever, vomiting, or decreased appetite or activity.
Some kids experience UTIs again and again — these are called recurrent UTIs. If left untreated, recurrent UTIs can cause kidney damage, especially in kids younger than 6. So it's important to know how to recognize the signs of these infections and get help for your child.
Types of UTIs
Common types of UTIs include:
- cystitis, the most common type of UTI, is a bladder infection that can occur when bacteria move up the urethra (the tube-like structure that allows urine to exit the body from the bladder) and into the bladder
- urethritis, when bacteria infect the urethra
- pyelonephritis, a kidney infection that can occur when infected urine flows backward from the bladder to the kidneys, or when an infection in the bloodstream reaches the kidneys
Related Conditions Associated With Recurrent UTIs
Recurrent UTIs are sometimes seen in conjunction with other conditions, such as:
- vesico-ureteral reflux (VUR), which is found in 30%-50% of kids diagnosed with a UTI and is a congenital (present at birth) condition in which urine flows backward from the bladder to the ureters (the thin, tube-like structures that carry urine from the kidney to the bladder) and sometimes reaches the kidneys. If the urine in the bladder is infected with bacteria, VUR can lead to pyelonephritis.
- hydronephrosis, which is an enlargement of one or both kidneys due to backup or blockage of urine flow and is usually caused by severe VUR or a blocked ureter. Kids with hydronephrosis are sometimes at risk of recurrent UTIs and may need to take daily low doses of antibiotics to prevent them.
But not all cases of recurrent UTIs can be traced back to these body structure-related abnormalities. For example, dysfunctional voiding — when a child doesn't urinate frequently enough or doesn't relax his or her muscles properly while urinating — is a common cause of UTIs.
Unrelated conditions that compromise the body's natural defenses, such as diseases of the immune system, can also lead to recurrent UTIs. In addition, using a nonsterile urinary catheter can introduce bacteria into the urinary tract and cause an infection.
Detecting Abnormalities
Although UTIs can be treated with antibiotics, it's important for your child's doctor to rule out any underlying abnormalities in the urinary system when these infections occur repeatedly.
Some abnormalities can be detected even before birth. Hydronephrosis, when it occurs as a congenital condition, can be detected in a fetus by ultrasound as early as 16 weeks of gestation. When hydronephrosis poses significant danger to the developing kidneys, surgery may be performed while the baby is in the womb; however, in most cases, doctors wait until after birth before treating the condition because almost half of all cases that are diagnosed prenatally disappear by birth.
Once a baby suspected to have hydronephrosis or another urinary system abnormality is born, the baby's blood pressure will be monitored carefully because some kidney abnormalities can cause high blood pressure. An ultrasound may be used again to get a closer look at the bladder and kidneys.
Diagnosis and Treatment
If your doctor suspects that your child may have an abnormality of the urinary tract, he or she may order tests to make an accurate diagnosis including:
Ultrasound
Using high-frequency sound waves to "echo," or bounce, off the body and create a picture of it, an ultrasound can detect some abnormalities in the kidneys, ureters, and bladder. It can also measure the size and shape of the kidneys. When an ultrasound suggests VUR, a voiding cystourethrogram (VCUG) or a renal scan (see below for descriptions of both) may be performed for further evaluation.
Renal scan (nuclear scan)
Radioactive material is injected into a vein and followed through the urinary tract. The material can show the shape of the kidneys, how well they function, if there is damaged kidney tissue, and the course of the urine. A small amount of radiation is received in the study and leaves the body in the urine.
Voiding cystourethrogram (VCUG or cystogram)
A catheter (a hollow, soft tube) is used to inject an opaque dye into the bladder. This X-ray test can diagnose VUR and identify problems with the bladder or urethra.
Cystoscopy
A cystoscope uses lenses and a light source within a tube inserted through the urethra to directly view the inside of the bladder. It's used when other tests or symptoms indicate a possible bladder abnormality.
Intravenous pyelogram
Opaque dye is injected into a vein and then X-rays are taken to follow the course of the dye through the urinary system. Although this test is still used sometimes, the renal ultrasound and renal scan have replaced intravenous pyelogram in most cases.
Because VUR can lead to kidney infection (pyelonephritis) and subsequent kidney damage, children with the condition must be monitored closely. Usually, surgery isn't necessary because many kids will outgrow the condition. Even in those who don't, surgery may be unnecessary because antibiotics are often successful in warding off UTIs.
The most common type of surgery to correct VUR is ureteral reimplantation, in which one or both ureters are reattached to the bladder to decrease backflow of urine from the bladder to the ureters and kidneys. Although the success of ureteral reimplantation is greater than 90%, only those who have recurrent UTIs while on antibiotic prophylaxis (preventive therapy) will be considered for surgery.
Blockages can interfere with normal urine flow, which serves to wash bacteria out of the urinary tract. Because severe blockages in the ureter or the urethra may ultimately lead to repeated kidney infections and kidney damage, they may require surgical intervention. Kidney stones are another source of blockage that may obstruct the path of urine.
When anatomical defects have been ruled out, antibiotics may be prescribed for months or even years to prevent recurrent infections.
The Future for Managing Recurrent UTIs
Doctors have started to use a less-invasive way to correct VUR than implantation. The procedure involves the injection of such materials as Teflon, Delflux, or collagen through a cystoscope. This procedure was considered experimental a few years ago, but is rapidly gaining wider acceptance.
Recent studies have found that women and children who get recurrent UTIs may lack certain immunoglobins (a group of proteins that fight infections). Some researchers are optimistic that a vaccine may be developed that could help boost production of antibodies that fight UTIs. A promising vaccine that would protect against E. coli (the most common bacterium that causes UTIs) is being tested.
Home Treatment
Additional things to consider to help prevent recurrent UTIs in kids:
Diet Modifications
Encourage kids to drink 8 to 10 glasses of water and other fluids per day. Cranberry juice is often suggested because it may prevent E. coli from attaching to the walls of the bladder. Always ask your doctor, though, if your child should drink cranberry juice because it can interfere with some medicines.
Multivitamins
Vitamin C acidifies the urine, making the environment less friendly to bacteria. Vitamins designed for kids are generally safe, but always ask your doctor before increasing the dose beyond the currently recommended daily allowance.
No Bubble Baths
Kids should avoid bubble baths and perfumed soaps because they can irritate the urethra.
Frequent Diaper Changes
Kids in diapers should be changed frequently to prevent stool from having prolonged contact with the genital area, which can increase the chance that bacteria will move up the urethra and into the bladder.
Proper Wiping Technique
In females, wiping from front to back after using the toilet will reduce exposure of the urethra to UTI-causing bacteria in the stool.
Cotton Underwear
Breathable cotton underwear is less likely to encourage bacterial growth near the urethra than nylon or other fabrics.
Frequent Bathroom Visits
Some kids may object to using the school bathroom or may become so engrossed in a project that they delay urination. Kids with UTIs should urinate at least every 3 to 4 hours to help flush bacteria from the urinary tract.
Follow-Up Visits
Your doctor may advise performing another urine culture after treatment of a UTI is completed to be sure that the infection has cleared.
When to Call the Doctor
As soon as you suspect a UTI in your child, it's important to contact your doctor.
If your child suffers from recurrent UTIs, consult a pediatric nephrologist or urologist who can perform a thorough evaluation and, if necessary, order tests for urinary system abnormalities. In the meantime, follow your doctor's instructions for treating a UTI.
 Rabies infections in people are rare in the United States. However, worldwide about 50,000 people die from rabies each year, mostly in developing countries where programs for vaccinating dogs against rabies don't exist. But the good news is that problems can be prevented if the exposed person receives treatment before symptoms of the infection develop.
Rabies infections in people are rare in the United States. However, worldwide about 50,000 people die from rabies each year, mostly in developing countries where programs for vaccinating dogs against rabies don't exist. But the good news is that problems can be prevented if the exposed person receives treatment before symptoms of the infection develop.  Polio (also called poliomyelitis) is a contagious, historically devastating disease that was virtually eliminated from the Western hemisphere in the second half of the 20th century. Although polio has plagued humans since ancient times, its most extensive outbreak occurred in the first half of the 1900s before the vaccination, created by Jonas Salk, became widely available in 1955.
Polio (also called poliomyelitis) is a contagious, historically devastating disease that was virtually eliminated from the Western hemisphere in the second half of the 20th century. Although polio has plagued humans since ancient times, its most extensive outbreak occurred in the first half of the 1900s before the vaccination, created by Jonas Salk, became widely available in 1955.  Conjunctivitis, commonly known as pinkeye, is an inflammation of the conjunctiva, the clear membrane that covers the white part of the eye and the inner surface of the eyelids.
Conjunctivitis, commonly known as pinkeye, is an inflammation of the conjunctiva, the clear membrane that covers the white part of the eye and the inner surface of the eyelids. 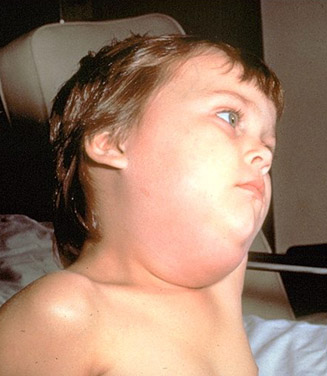 Mumps is a disease caused by a virus that usually spreads through saliva and can infect many parts of the body, especially the parotid salivary glands. These glands, which produce saliva for the mouth, are found toward the back of each cheek, in the area between the ear and jaw. In cases of mumps, these glands typically swell and become painful.
Mumps is a disease caused by a virus that usually spreads through saliva and can infect many parts of the body, especially the parotid salivary glands. These glands, which produce saliva for the mouth, are found toward the back of each cheek, in the area between the ear and jaw. In cases of mumps, these glands typically swell and become painful.